One of the first warning signs people expect in a medical crisis is pain. Sometimes, pain is even the deciding factor in whether or not a person decides to seek medical treatment. But in the case of retinal detachment – a serious eye condition that can lead to permanent vision loss if left untreated – there’s no pain.
While on the surface that may seem like a good thing, ophthalmologists say the painlessness associated with the condition is more of a curse than a blessing, as it sometimes keeps people from seeking treatment as soon as they should.
“Patients think, ‘If I have a retinal detachment, I should have pain,’” Dr. Carlos Martinez, an ophthalmologist with Eye Physicians of Long Beach, told the Business Journal. Martinez is also the president of the Los Angeles County Medical Association’s Long Beach District, and is a fellow of several medical organizations, including the American Academy of Ophthalmology.

(Dr. Carlos Martinez, an ophthalmologist with Eye Physicians of Long Beach. Photograph by the Business Journal’s Evan Patrick Kelly)
“Because there is never any pain associated with it, some people will wait and say, ‘Well I am busy today. If it doesn’t get better by tomorrow, I will call in and getan appointment for next week,’” Dr. Fox Boswell, an ophthalmologist with Bixby Knolls-based South Coast Retina Center, said. “Nobody looks forward to pain. But, in this case, it would be a nice warning sign. People would come in right away if their eye hurt. It’s human nature.”
Retinal detachment occurs when the retina – the light-sensitive tissue lining the eye that captures images filtered through the lens and cornea – starts peeling away from the wall of the eye. There are three kinds of retinal detachment, but by far the most common is rhegmatogenous retinal detachment, which is caused by a tear in the retina.
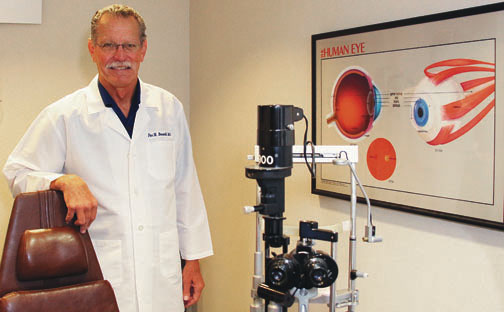
(Dr. Fox Boswell, an ophthalmologist with South Coast Retina Center. Photograph by the Business Journal’s Evan Patrick Kelly)
Dr. Henry Wiley, an ophthalmologist and staff clinician for the National Eye Institute, said this type of retinal detachment occurs in between 10 to 20 people per 100,000 people per year.
Tears in the retina are most often caused either by a trauma (such as eye surgery, a car accident, a blow to the head or an object piercing the eye) or by the separation of the vitreous gel, a clear fluid inside the eye, from the retina. In cases where rhegmatogenous retinal detachment is caused by blunt trauma, between 20 to 40 percent of cases occur in people who have had previous eye surgery, according to Wiley.
“The most common surgery in that regard is cataract surgery. . . . People would quote you somewhere in the range of 1 to 2 percent risk of retinal detachment following cataract surgery,” he explained to the Business Journal.
The separation of the vitreous gel from the eye eventually occurs in everyone, because that gel liquefies as a function of age. While this only occurs in about 10 percent of people under the age of 50, it occurs in at least one eye for 60-plus percent of people over the age of 70, Wiley said. When the vitreous separates from the eye, it sometimes tugs on the retina, causing a tear.
When the retina tears, fluid builds up behind it, slowly pushing it away from the eye wall. Warning signs of a tear typically occur in the form of a sudden onset of floaters – tiny proteins floating around inside the eye that may look like gray or black bubbles, specks, ball and chains, or cobwebs – and flashes of light.
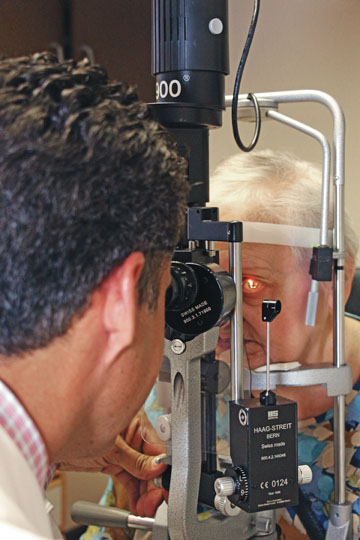
(Dr. Carlos Martinez, an ophthalmologist with Eye Physicians of Long Beach examines a patient to determine if she has a retinal tear or detachment. In either situation, it is important to act quickly to ensure the problem doesn’t progress to the point that vision is lost. Photograph by the Business Journal’s Evan Patrick Kelly)
This is precisely what happened to former Long Beach Mayor Bob Foster about two months ago.
“It’s not fun,” he said in a phone interview with the Business Journal. “I saw the flashes and large floaters, and it was also a little like looking through a slightly dirty window,” Foster recalled.
Because he knew these could be early warning signs of retinal detachment, he set up an appointment to see Boswell, who could not see a tear but told Foster his vitreous was liquefied to a large degree, which may have been causing his symptoms.
Over the following weekend, matters suddenly took a turn for the worse.
“As I sat down to dinner with some friends of mine, all of the sudden the eye got a huge amount of floaters. It looked like lattice work,” Foster said. “The vision became much more impaired, and it got worse as the night went on.” He scheduled an appointment to see Boswell the following Tuesday.
What happened next caused Boswell to make time for Foster sooner than that. On Saturday, Foster noticed a shadow in his peripheral vision, a key warning sign of a retinal detachment. “Sure enough, I had both a tear and a detachment,” he said. Boswell saw him Sunday night, which happened to be Father’s Day.
Martinez recommended seeing an eye specialist as soon as a sudden onset of floaters or flashes occur, just like Foster did. While these may simply be signs of the vitreous separating from the retina, they are also indicative of a retinal tear, which can be mended before the retina detaches if it is caught early. “If they laser the tear, you essentially weld the retina back to the eye and it has a smaller chance of detachment,” he said.
Some people, however, do not experience flashes or floaters when they have a retinal tear or the beginnings of retinal detachment, Boswell pointed out. “Once in awhile, somebody will just notice a shadow, just all of the sudden like somebody drew a curtain,” he said.
Once a retinal tear progresses to a retinal detachment, the detachment usually starts along the periphery of the retina, where it is typically weaker. In people with myopia, which is near-sightedness, this point of the retina is even weaker because their eyes are longer, making the retina more stretched and thin. This makes people with myopia more at risk for retinal detachment, Meyer noted.
If a retinal detachment is treated before it advances to include parts of the retina closer to the center of the eye, “you almost always get your peripheral vision back,” Boswell said. “But the central retina, which is called the macula, is more sensitive to being detached from the eye wall. Those light receptors [located there] get their nutrients and the exchange of visual pigment with the eye wall, and when they detach they start to deteriorate more rapidly and they don’t come back as well,” he explained.
“When you allow retinal detachment, which usually starts out in the periphery, to go all the way to the macula, the outcomes are fairly poor,” Martinez said. “It is really hard to restore vision.”
In Foster’s case, the detachment was caught early enough that he regained good vision following treatment. Boswell treated Foster by first numbing his eye and then draining the vitreous fluid from it. He then used cryogenic tool to freeze the point of tearing, which created scar tissue that the retina adhered to.
“Then what they do is the most amazing thing to me. They put gas in your eye,” Foster said. “The pressure from the gas forces the retina back in place, and the gas stays in your eye on average between three to six weeks. . . . Who the hell ever thought of that, I don’t know.” Gas is typically only used in instances where the tear is towards the top of the eye, because gas moves upward, Boswell noted.
In some instances, it is only necessary to insert gas into the eye and heal the tear with a laser, Martinez said. A more invasive procedure involves attaching a small band to the eye to hold the retina in place.
“My vision has come back,” Foster said. “I had 20/25 vision in that eye. The best I can muster [now] is probably 20/50,” he said. “Sometimes my vision is distorted. Objects in that eye appear somewhat smaller, but over time, that should correct.”
The success rate of repairing retinal detachments with gas is 70 to 75 percent, Boswell said. Other procedures typically have a 90 percent success rate.
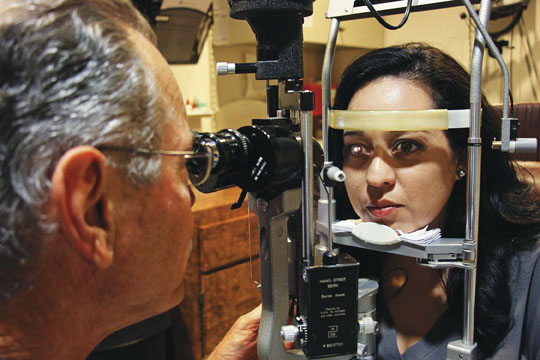
(Dr. Fox Boswell, an ophthalmologist with South Coast Retina Center in Bixby Knolls, recently treated former Long Beach Mayor Bob Foster for a retinal detachment. Foster said his vision is recovering well. Here, he examines a patient who may have a retinal tear. Photograph by the Business Journal’s Evan Patrick Kelly)
In addition to trauma, aging and myopia, other risk factors for rhegmatogenous retinal detachment include a family history of retinal detachment and certain eye diseases such as uveitis, lattice degeneration and retinoschisis, according to Martinez. “It is more common in people above 40. It is more common in men and it is more common in whites than African Americans,” he added.
Foster emphasized the importance of seeing an eye specialist soon after experiencing warning signs. “I know one guy whose son kept saying, ‘It’s no problem, it’ll go away.’ Well, now he has permanent loss of peripheral vision,” Foster said. “So you really have to get at it very quickly.”
