While advances in medicine have enabled more people to live longer, the rising prevalence of Alzheimer’s disease and other dementias have prompted the need to explore new therapeutic and preventative strategies, according to researchers and health officials.
As the baby boomer generation advances in age, people in the United States and abroad are becoming more susceptible to developing Alzheimer’s disease, a degenerative brain disease that most commonly begins with memory loss and eventually leads to death.
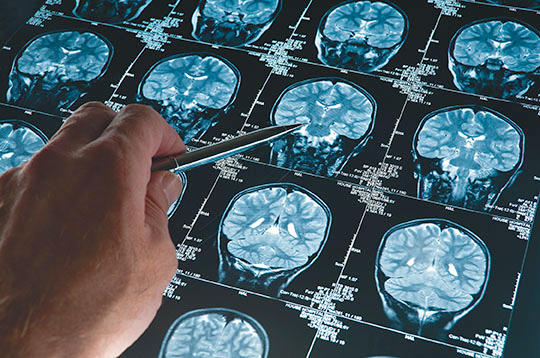
Magnetic resonance imaging (MRI) scans of the brain are often used to diagnose Alzheimer’s disease before symptoms of memory loss are present in a patient. (Photograph courtesy of New York University’s School of Engineering)
According to a report called “2015 Alzheimer’s Disease Facts and Figures” from the national Alzheimer’s Association released earlier this year, there are an estimated 5.3 million people in the United States living with Alzheimer’s disease, the sixth leading cause of the death in the country.
By the middle of the century, the number of people with the disease is expected to triple to 16 million, according to the report. In the next decade, 19 states in the country are expected to see a 40 percent or greater growth in the number of people with Alzheimer’s disease.
“The prevalence is rising dramatically, but that very much follows the demographics of our society,” said Dr. Debra Cherry, a clinical psychologist and executive vice president of the Alzheimer’s Association California Southland Chapter. “Our society is aging, and the No. 1 risk factor for Alzheimer’s disease and many other dementias is age.”
The rise of Alzheimer’s disease comes as the prevalence of other chronic diseases, such as heart disease, diabetes and cancer, has declined thanks to medical advancements.
In fact, according to the report, deaths from Alzheimer’s disease increased 71 percent from 2000 to 2013 while deaths from other major diseases, including heart disease, stroke, breast and prostate cancer and HIV/AIDS, have decreased.
The Alzheimer’s Association estimates that, unless something is done, costs associated with Alzheimer’s disease will rise to more than $1.1 trillion by 2050, with costs to Medicare increasing over 400 percent to $589 billion.
According to Cherry, as baby boomers survive into their late 70s and 80s – the age group with the greatest number of people with Alzheimer’s disease – more people are becoming at risk of developing the disease, and multiple clinical trials are underway in search of preventative measures and new interventions.
“People are living longer and, as they live longer, they are becoming more susceptible to Alzheimer’s and related dementias,” Cherry said. “That’s because they’re surviving other chronic diseases. It’s a public health phenomenon.”
Dr. Roberta Diaz Brinton, a neurologist, leading researcher of Alzheimer’s disease and professor at the University of Southern California’s (USC) School of Pharmacy who chairs the Alzheimer’s Association California Southland Chapter’s Medical & Scientific Advisory Council, said symptoms of the disease involve loss of short-term memory because an individual is unable to encode new information.

Dr. Roberta Diaz Brinton, a neurologist and leading researcher of Alzheimer’s disease at the University of Southern California’s (USC) School of Pharmacy, continues to lead research and clinical trials to discover new therapeutic strategies in treating Alzheimer’s disease. (Photograph courtesy of USC)
The disease eventually progresses to where a person might not be able to remember what happened yesterday or last week. Persons with the disease may also exhibit an inability to plan an event or solve problems. They might also have difficulty understanding where they are or may become confused in unfamiliar places, she said.
Furthermore, Alzheimer’s disease, which eventually leads to death after neurons in the brain die, often goes undiagnosed. In fact, only about half of all people living with the disease have ever been diagnosed, according to the Alzheimer’s Association’s report.
The difficulty in diagnosing the disease, Brinton explains, is that symptoms of Alzheimer’s disease, which are memory problems, are often confused with normal aging and the individual and family members might make adaptations to accommodate such problems.
Oftentimes, only when a person’s memory loss becomes “intrusive” on the family does proper diagnosis take place. Individuals also might never receive brain imaging because the technology might not be available or because of a person’s health care situation, she said.
An important advancement in understanding the disease, Brinton said, is that the National Institute on Aging (NIA) now acknowledges that Alzheimer’s disease is not a single disease but is caused by a “constellation of risk factors.”
With the exception of rare cases (an estimated 1 percent or less) that develop as a result of gene mutations, Alzheimer’s, like other chronic diseases, develops as a result of multiple factors, the Alzheimer’s Association noted.
Women, for instance, are found to be more at risk of developing the disease mainly because they tend to live longer than men and age is the No. 1 risk factor for the disease. However, being a female isn’t the only reason a person might develop the disease, Brinton said.
Understanding the complexity of how Alzheimer’s develops in the brain allows researchers to broaden their approach for therapeutic strategies, opening up opportunities for “precision medicine,” she said.
Though there has yet to be found any therapeutic strategies that stop the disease’s progression or change the underlying course of the disease once it develops, current interventions may alter symptoms or slow onset of the disease.
“For the first time in about 15 years, I’m at the point of saying . . . we may have something within the next five years that makes a difference,” Cherry said.
While the average age of diagnosis is around 75, about the time a person starts exhibiting major lapses in memory, recent advances have shown evidence of Alzheimer’s developing in the brain up to 10 years or more before clinical symptoms emerge.
The main hypothesis behind the pathology of Alzheimer’s appears to be that the enzyme “gamma-secretase” disrupts the processing of amyloid precursor protein (APP) in the brain, creating instead a short fragment of APP known as beta-amyloid. The accumulation of clumps of this sticky protein fragment in the brain (called amyloid plaques) triggers the disruption and destruction of nerve cells that causes Alzheimer’s disease.
Dr. Omid Omidvar, a neurologist and member of the Long Beach Memorial, Miller Children’s & Women’s Hospital Long Beach and Community Hospital Long Beach medical staff, said via e-mail that therapeutic arsenals currently available remain “very limited,” however researchers are actively searching for disease modifications.

Dr. Omar Omidvar is a neurologist and member of the Long Beach MemorialCare Health System who practices at the Southland Neurologic Institute in Long Beach. The institute collaborates with a clinical research center called CNS Network that conducts clinical trials for new therapeutic strategies in treating Alzheimer’s disease. (Photograph courtesy of Long Beach MemorialCare Health System)
He added that there are multiple therapies in different phases of clinical and preclinical development attempting to target beta-amyloid through the use of certain drugs.
“It is thought that drugs that either could inhibit this enzyme or products that could passively immunize the brain against this toxic protein could reduce beta-amyloid accumulation, which may play a role in various neurodegenerative disorders,” he said.
Omidvar also practices at the Southland Neurologic Institute located at Douglas Park in Long Beach. He said the institute is in active collaboration with a leading clinical research center called CNS Network, also located in Long Beach, offering the local community access to a large spectrum of clinical trials for researching Alzheimer’s disease.
He said researchers are developing therapies that also target “tau,” the protein involved in “tangles” being developed in the brain that result in nutrients and other essential supplies being unable to move through brain cells, which eventually die. Omidvar said some researchers are hoping to reduce brain pathology and even regenerate damaged cells.
Some trials, however, have yet to be conducted with humans. For instance, researchers at The University of Queensland in Australia claim to have developed a non-invasive Alzheimer’s treatment technique using ultrasound technology.
In a series of experiments on mice bred to develop Alzheimer’s, regular ultrasound scans triggered the brain to break up brain plaques and showed signs of reversing memory loss in the mice. The achievement has been hailed as a “breakthrough.”
In an e-mail to the Business Journal, Prof. Jürgen Götz, foundation chair of dementia research at The University of Queensland and inaugural director of the Clem Jones Centre for Ageing Dementia Research at the Queensland Brain Institute, said that it’s uncertain when this type of treatment might be tested on humans mainly because of safety issues, particularly for long-term treatment in aged individuals. However, he added that ultrasound has been used to open the blood-brain barrier for the first time non-invasively to treat cancer.

Prof. Jürgen Götz, foundation chair of dementia research at The University of Queensland and inaugural director of the Clem Jones Centre of Ageing Dementia Research at the Queensland Brain Institute in Australia, was part of a recent study to develop a non-invasive treatment for Alzheimer’s disease using ultrasound technology to break up brain plaques in mice. (Photograph courtesy of Prof. Jürgen Götz)
Still, Brinton said that, while such therapeutic approaches may have promise, they still aren’t tackling the issue of why the brain is forming plaques in the first place.
Omidvar said that, since Alzheimer’s disease is a progressive and chronic condition that may be present before symptoms arise, there are many clinical trials attempting to prevent the formation of beta-amyloids in healthy or mildly affected persons.
Lifestyle modifications, if started early enough, could significantly delay the onset of the disease, he said. In addition, researchers have found that people who stuck to a healthy diet with foods such as berries, leafy greens and fish, had a drop in risk for Alzheimer’s disease, he said.
Treating underlying sleep disorders like sleep apnea and treating metabolic disorders like diabetes and hypertension are also important steps people can take, Omidvar said.
Daily physical and social activities, avoidance of head injuries and concussions (especially during high school and college sports) as well as taking certain natural supplements may also result in delaying or even fully preventing the disease, he said. Others have noted that cognitive stimulation, such as playing brain games, may also help delay onset of Alzheimer’s disease.
