Eight weeks ago today, August 15, I was diagnosed with breast cancer. Three weeks ago, I had surgery to remove the cancer and verify it hadn’t traveled beyond my breast. Today I’m cancer free, although I have opted to undergo radiation to lower the risk of recurrence. Also, I’ll be on hormonal therapy (a pill a day) for about five years. I feel very fortunate. And surprised. Surprised to learn my experience wasn’t a miracle of medicine but a fairly common breast cancer recovery experience, perhaps even more common than the graver, more difficult ordeal I have always associated with a breast cancer diagnosis. So I’d like to share my experience, hoping that readers might take heart and benefit from what I learned.
Breast Cancer Is Not Always A Grave Diagnosis
My attitude toward breast cancer had always been that it is a dire and tragic diagnosis. I had only ever heard of women who had endured significant surgeries, long periods of debilitating chemotherapy and radiation, and – if they survived – a future where the specter of breast cancer would always lurk. I fully realize that, sadly, breast cancer can play out this way, and there are readers who understand this far more deeply than they’d like to. What I learned, though, is that this isn’t the typical profile of breast cancer. My experience is quite common and, with early detection and improved treatments, becoming more so every day.
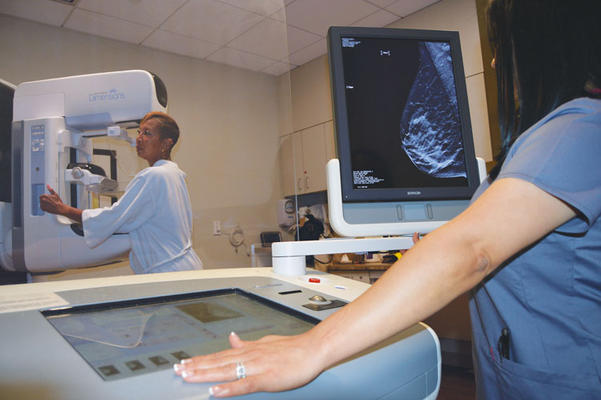
A nurse at the MemorialCare Breast Center in Long Beach reviews a 3-D image of a patient’s breast tissue taken by tomosynthesis. This process, rather than traditional 2-D imaging, allows health care professionals to examine a cross-section of breast tissue and more easily spot cancer. Dr. Angela Sie, breast imaging medical director at the center, explained that the difference between traditional 2-D imaging and tomosynthesis is similar to trying to peer through a book cover rather than opening up the book and looking at it one page at a time. The center is located within the Todd Cancer Pavilion on the campus of Long Beach Memorial Medical Center. (Photograph by the Business Journal’s Larry Duncan)
Early Detection Is The Key
Early detection is oh so important. It means the difference in the size of the tumor and the likelihood of cancer cells migrating outside the breast. Frequent self-examinations are important, but they don’t replace mammograms, which can detect tumors too small to feel. The reason I was able to have a lumpectomy (removal of the tumor and a surrounding margin of tissue) was because the cancer was detected during a routine mammogram when it was still very small – 0.6 cm, about the size of a small pea, too small to feel with self-exams. Otherwise, I would have been looking at breast removal, with reconstruction (breast implant) at the same or a later time (which I would have willingly dealt with). Early detection also meant the cancer cells didn’t have the chance to travel to the lymph nodes in my armpit and elsewhere in my body, which would have meant chemotherapy, lengthier recovery and perhaps a poorer prognosis.
Any Woman Can Get Breast Cancer
While the diagnosis of breast cancer may not be, across the board, as grave as I had thought, I learned it is more prevalent than I had realized (about one in eight women will get breast cancer), even among those of us who consider(ed) ourselves low risk. I, in fact, had considered myself basically “no risk.” After all, there is no history of cancer in my family, I’ve made it past age 60 safely, I don’t smoke, I’m physically active, and I’m pretty much the picture of health. Couldn’t happen to me, right? Wrong. We don’t know what causes breast cancer, and you – yes, you – might get it. According to the California Department of Public Health, 80% of women who develop breast cancer are over 50 years old. And only 20% to 30% of women who get it have family members with the disease. (Men can also contract breast cancer, accounting for about 1% of all cases.) So, please don’t be complacent – get your mammogram.
See It For What It Is
When I first got The Diagnosis, admittedly, I felt a quick shock flutter through my body. Within a few moments, though, I felt peaceful, saying to myself, “OK, this is the situation. I’ll do what I need to do. Everything will work out.” And I knew that to be true. I did not relate to a grave outcome, and I wasn’t going to “go there.” I understood the importance of staying centered in that attitude and not allowing the fears of others, however well intended, to seep in. Plus, I didn’t want to hear myself endlessly talking about it. If things turned more serious, I would deal with it and have loving, positive support around me. Naturally, I would need to tell my daughters, my siblings and a few friends who I see often. (Try as I might, I just can’t keep a secret when it comes to my own business.) After consulting with the surgeon a few days later and getting an idea of my options, I basically said, “I have some news. It’s not as bad as it sounds, and things will turn out fine. I have a small cancer in my breast, which needs to be removed. It’s unlikely I’ll need chemotherapy, and I may not even need radiation.” There was a little more detail, but that’s the gist of it. My family and friends were supportive and, perhaps taking their cue from me, not unduly alarmed.
Pick Health Care Providers With A Positive Attitude
One friend advised me to get a second opinion, and I remember wondering: Why a second opinion? I have a cancerous tumor and it needs to come out, and I’ll either need chemotherapy or I won’t. Well, he was right. I accidentally got a second opinion because, when I asked for the earliest surgery date available, I was assigned to a different surgeon than the one I had originally consulted with. The first surgeon had seemed competent and caring but had a somewhat somber view, citing the necessity for 5-6 weeks of radiation and advising me to decide whether I wanted to have my breast removed and reconstructed, or conserved. The second surgeon said radiation may not be necessary and that breast conservation was a no-brainer, that only a small amount of tissue would be removed and the breast would fill itself in over time. (Even a couple of days after surgery, my breast looked pretty normal except for slight bruising and the incision.) Also, after one appointment with a most disagreeable medical oncologist, I immediately requested another one going forward. And, yes, I did end up opting for radiation (five days a week for three weeks), to reduce the risk of recurrence from just below 10% to about 2% to 3%.
I’m just one person with one breast cancer experience, but I learned a few lessons here: You may not be able to prevent breast cancer if it’s got your name on it, but you can try to head it off at the pass. Get regular mammograms and deal with it early. Keep a realistic, positive view. Be choosy about how and with whom you share your experience, including health care providers. Keep living your life as fully as you can.
(Pat Flynn has previously served as a copy editor and guest columnist for the Business Journal. Comments about this article may be sent to her attention at: info@lbbj.com)
